“Understanding Biocompatibility Before Dental Treatment” by Dr. Blanche D. Grube
One of the things I have noticed over the many years of my dental career is that “ALL” dentists think that they are the best dentist in their community, state, or maybe even the country. Yet there is something that many of these dentists are completely unaware of when they examine a patient, come up with a diagnosis, and then formulate a treatment plan. To assist in making a diagnosis they may have the best X-ray equipment available and study the X-rays with a magnifying lens. They may even have the latest 3D X-ray machine which gives the doctor a view of the whole head, inside and out, and in every direction imaginable! Most patients get a real kick out of seeing their own skull, even if it is a little bit scary looking. While these new 3D X-rays are not as good as the two-dimensional X-rays for the detection of cavities, when it comes to looking for bone pathology and abscesses, these state-of-the-art X-rays provide the doctor with views that make the old two-dimensional X-rays seem archaic.
Nearly all dentists wear optical lenses that magnify everything within the mouth. All these technological advances make developing a treatment plan based on a very thorough exam much easier for the dentist and the patient. But most often, the one critical part that is missing in the treatment plan, is the presentation and decision of what kind of dental materials the dentist will use and be permanently placing into the patient’s mouth, which can be the most hostile environment in the human body. This is extremely important because the dental materials used, will ideally remain for many years, or even better, for the rest of the patient’s life!
How does the dentist decide what material to use? Do they simply choose a dental material that is on sale that week? Is it a “new” material that a dental rep recently brought into their office? Sometimes, these free samples come with several color brochures to convince the dentist that buying this product is akin to walking on the beach with a beautiful healthy-looking partner next to them.
I once purchased a new laser because I truly believed that it was the best laser on the market for the surgical procedures I perform. After the purchase, I was told that I won an opportunity to drive a new BMW racecar around the racetrack in California. I still haven’t been able to figure out what a surgical laser has to do with racetrack driving. I said “no thanks” to the offer, besides, I have proof that I already drive too fast, according to the nice state trooper who wanted me to live longer by making me pay a fine so large, that I would remember it the next time I wanted to speed.
So, back to our question, how do dentists decide which dental material is best for the patient and best for a particular restorative application? While biocompatibility is the new “buzzword” in dentistry what does it really mean? In simple terms, it means that the material being used should not have a negative impact on the health of the recipient.
Most dentists are not even aware that there is a laboratory that can help them to decide what materials are going to be least reactive to their patients’ bodies. You may have noticed that I said “Least” reactive and not “Non-Reactive”. The reason is because any foreign material placed into someone’s mouth is going to be recognized as just that, foreign. The body is obligated via its’ immune system to recognize anything that is not part of the body and elicit an immune response. In other words, anything that is not SELF has the potential to be reactive to the patient. The body WILL react to a greater or lesser extent depending on the material’s level of safety and biocompatibility. It is important to be aware that the level reaction to the foreign material is often not evident.
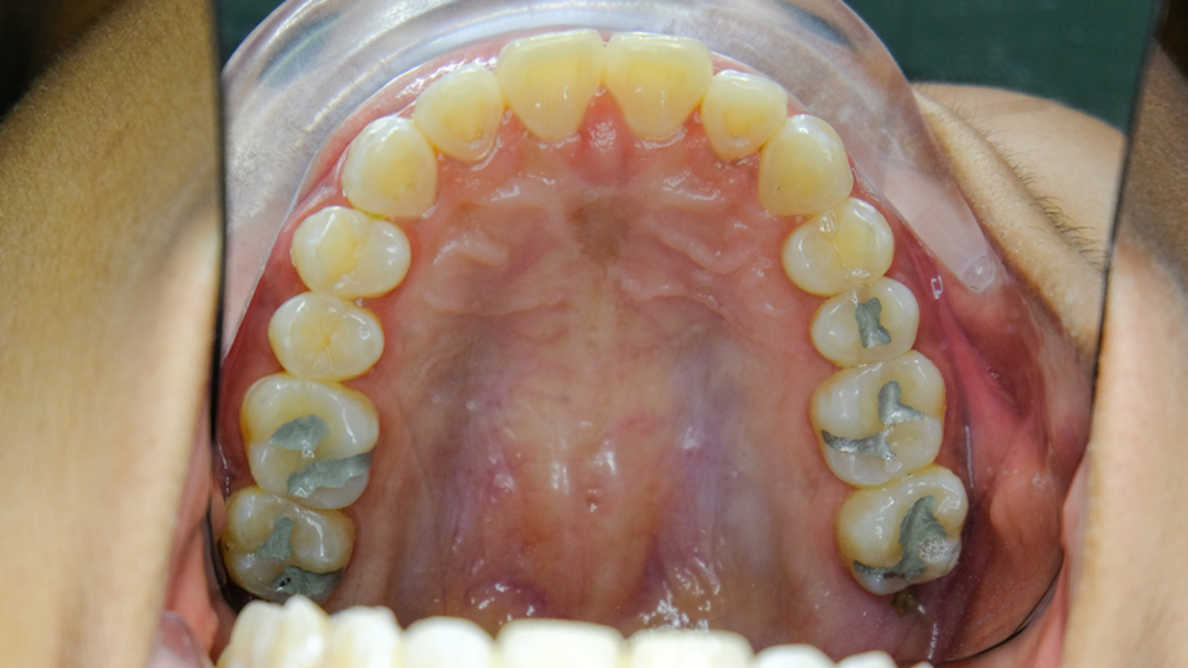
For example, most people are unaware of the changes that have occurred and continue to occur in their body after a mercury amalgam filling is placed into their mouth. Mercury is the most toxic, non-radioactive element on the planet. The immunological and physical effects that may take place can occur slowly over time and are cumulative, making it difficult for the person to make any connection between the placement of the filling and their declining health. Note: this also applies to the safe removal of mercury amalgam fillings and the subsequent placement of an alternative restoration. If the dentist is truly interested in restoring or maintaining the patients’ health then a Serum Biocompatibility Test should be performed prior to the placement of new fillings, crowns, or bridges. A blood sample is collected, the serum is separated off, frozen and sent to Biocomp Laboratories in Colorado Springs. The lab analyzes the serum to determine the patient’s levels of dental material reactivity.
As I previously stated, the immune system, meaning the white blood cells, is obligated to respond to anything that it recognizes as non-self. If the white blood cells recognize a dental material as something that is dangerous for the survival of the body, then those white blood cells will produce a specific protein response called agglutination, or clumping, of the white cells around the specific material. At Biocomp Laboratories the serum is individually exposed to 78 unique ‘components’, which are common ingredients found in dental materials. If the immune system responds strongly, the observed reaction would appear very opaque, turbid and viscous in appearance and it would be categorized as a “Highly Reactive Material”. If the immune system does not respond as much to the dental component, then the reaction would appear somewhat opaque and slightly clumpy. This material would be labeled as a “Moderately Reactive Material”. Finally, if the sample exhibits a relatively clear appearance, this material would be labeled as a “Least Reactive Material”. An optical density scanner quantifies the intensity and extent of the protein agglutination and provides a ‘reactivity level result’. Finally, each of the reactivity levels are extrapolated to the 9500+ specific dental products in our database. For example, if a person is determined to be highly reactive to copper, then any product in our database, regardless of the dental usage, that contains copper will be categorized as a ‘Highly Reactive’ product in the patient’s report. As I mentioned before, there is no such thing as foreign material being NON-reactive. The immune system will recognize it as NON-SELF and respond appropriately. After this test is complete, a full report listing 9500+ dental products will be sent to the dentist and/or the patient.
The report is complete with the product names, manufacturer, and contact information of the manufacturers so that it is easy for the dentist to choose what materials are best for that specific patient. Each product in the report is categorized by dental usage (ex. composites, porcelain & ceramics, etc.), and sorted by determined reactivity levels. Further, Biocomp Laboratories provides a complete A to Z listing of all 9500+ products, also sorted by determined reactivity levels. Practitioners can always request product research and addition to the database, if needed.
I’ve never really been able to figure out why anyone would not want to have this test done, except not having the knowledge of its existence. If a dental material reactivity test is not done prior to having the dental work completed, then the dentist is really just guessing. They are guessing that the patient’s immune system will be OK with that material. To that, my only answer is “DON’T GUESS…GET THE TEST!”
Blanche D. Grube, DMD has been practicing dentistry for over 40 years. Her practice, the Huggins-Grube Dental Center, is located in Scranton, PA. Mentored by the late Dr. Hal Huggins, Dr. Blanche continues to train and educate dental practitioners worldwide on The Huggins-Grube Protocol and The Full Dental Revision – the safest method of removing and replacing dental restoration materials.
About Biocomp Labs
Dental toxicity can occur when foreign materials are placed in a patient’s mouth – this can cause the immune system to react and reject the restoration. Biocompatibility testing allows patients and practitioners to learn about and avoid dental toxicity by avoiding the use of reactive materials in the mouth. Biocomp Labs offers biocompatibility testing to patients and their dental practitioners in order to determine the patient’s reactivity to 78 different components used in common dental materials.
References:
- Pauwels R. History of Dental Radiography: Evolution of 2D and 3D imaging Modalities. (2020) Medical Physics International Journal. http://mpijournal.org/pdf/2020-SI-03/MPI-2020-01-p235.pdf
- Vazquez-Tibau A, Grube BD, DMD, Biocompatibility in Dentistry: A Mini Review. (2021) Mod Res Dent. 6(4). https://drblanchegrube.com/wp-content/uploads/2021/07/Biocompatibility-in-Dentistry-A-Mini-Review.pdf
- Anjum AS, Ganapaththy D, et al. Mercury leaching from amalgam. (2019) Drug Invention Today. Vol. 12. Issue 10. https://www.researchgate.net/profile/Kiran-Pandurangan/publication/343961736_Mercury_leaching_from_amalgam/links/5f49f80692851c6cfdf7e8b9/Mercury-leaching-from-amalgam.pdf
- Shahi S, Ozcan M, et al. A review on potential toxicity of dental material and screening their biocompatibility. (2019) Toxicology Mechanisms and Methods, DOI: 10.1080/15376516.2019.1566424
- Bapat RA, Parolia A, et al. Recent update on potential cytotoxicity, biocompatibility and preventive measures of biomaterials used in dentistry. (2021) Biomaterials Science. Issue 9
- Hosseinpour S, Gaudin A, et al. A critical analysis of research methods and experimental models to study biocompatibility of endodontic materials. (2022). International Endodontic Journal. Vol.55, Issue 52; 346-369.