Everyone knows that going for an annual checkup is good for your health. These checkups can provide you with information and discover potential health problems before they can develop into something serious. What has been the most overlooked area as to where many of these health problems actually start, is the mouth! Evidence-based science has confirmed that oral health, good or bad, is a determinative factor of whole-body health. Unfortunately, there has been an enormous disconnect between what is going on in the mouth and its connection to the rest of the body among medical doctors and dentist. Thankfully this old paradigm is changing, at least among doctors of integrative medicine, holistic health, and biological dentistry.
While there are many diseases that have been linked to oral health problems, we will focus our discussion on cardiovascular disease and stroke. To put these diseases into perspective, it is important to see just how pervasive they are not just in the United States, but also globally. Cardiovascular disease is the “big umbrella” for all types of diseases that affect the heart or blood vessels, including coronary heart disease (clogged arteries), which can cause heart attacks, stroke, heart failure, and peripheral artery disease.
In 2019, cardiovascular disease was identified as the leading cause of death worldwide, or about 17.9 million people representing 32% of all global deaths. Curiously in the information published by the World Health Organization (WHO) on cardiovascular diseases, there was no mention of oral health as a risk factor, nor as a preventive measure, even though this link has been well established in the scientific literature. The WHO does, however, mention that these diseases occur significantly more in low- and middle-income countries.
The Center for Disease Control and Prevention (CDC) has identified heart disease as the number one cause of death in the United States for men and women. Just like the WHO, it is tragic that the CDC doesn’t list poor oral health as a significant risk factor for heart disease. We need to ask ourselves why, when clearly this is well established in the scientific literature and why is it that cardiologists are one of the very few doctors who tell patients that they must see a dentist to make sure the patient doesn’t have any dental infections prior to any heart intervention therapy.
The separation between medical doctors and dentists is a very common problem when addressing patient health, not just for cardiovascular diseases, but also for other common diseases. The patient is left in the never-ending loop trying to discover the root cause of their disease, while medical doctors recommend extraordinary measures, such as surgery to “fix their problem”. Regrettably, this option doesn’t address the actual cause of the health problem that could have possibly been solved by addressing what is often a dental-related solution.
If a diet low in sugar and good oral hygiene is not followed by daily brushing and flossing to remove the plaque, tartar will form, which then, can only be removed by a dentist or dental hygienist. The longer dental plaque and tartar are on the teeth, the more harm they can cause. The first stage of periodontal disease is called “gingivitis” when the gums become red, swollen, and bleed easily. Luckily, this can be reversed and there is no bone loss or tissue loss that holds the teeth in place. Periodontitis is the result of untreated gingivitis that affects both the periodontal ligaments and bone surrounding teeth causing bacterial toxins to spread and, in this case, if left untreated, may end in tooth loss.
What happens when oral hygiene is neglected? Bacteria will take over… There have been about 800 different bacterial species that have been identified in dental plaque. These pathogens include both Gram-negative and -positive members, such as Treponema denticola, Tannerella forsythia, Prevotella intermedia, Agregatibacter actinomycetemcomitans, Campylobacter rectus, Eubacterium timidum, Parvimonas micra and Porphyromonas gingivalis. These pathogens have been linked to various heart problems. Bacteremia is understood as a transient rise of microorganisms in the blood and can result from both non-surgical and surgical dental procedures. It has been found to be a key factor of infective endocarditis in patients who are predisposed to cardiac disease or have a compromised immune system.
Some of the same bacteria that have been mentioned above are also found in endodontically treated teeth or root-canal-treated teeth. The evidence-based scientific literature shows many other common diseases, besides cardiovascular diseases, including cancer that has also been linked to the bacteria found in root canal-treated teeth.
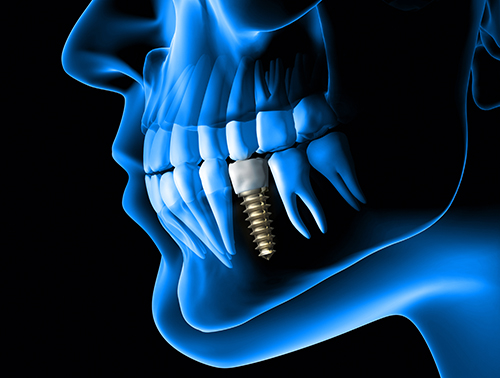
Another common dental procedure is the placement of dental implants, which has been growing over the last twenty years. Millions of implants are placed each year around the world. Bacteremia is also an issue with dental implants due to the invasiveness of the procedure.
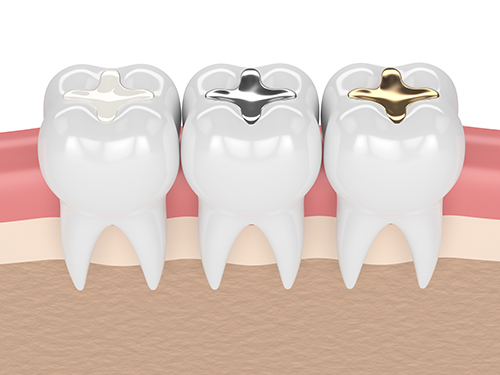
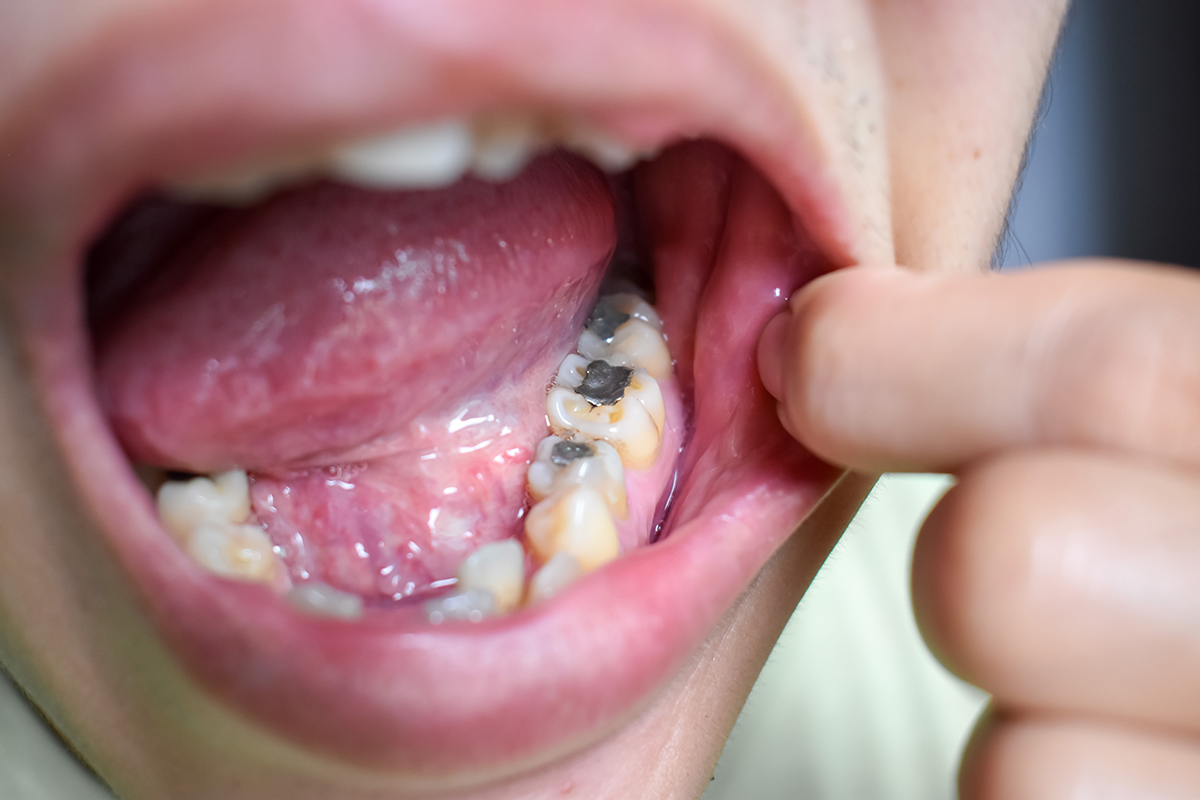
Regarding dental materials and their relationship to heart problems is the toxic mercury dental amalgam, one of the most common and most pervasive dental materials that have been used for almost 200 years!
With all the supporting scientific evidence that is available, we truly believe that the first place to look when wondering about the cause of a health problem is in the mouth, not only for heart problems but for any type of health challenges that a patient may be facing.
Do you know what’s in your mouth?
The DNA ConneXions® Propensity test panel identifies 19 of the most common bacterial species. This test not only identifies species involved in periodontal diseases, but also those microbes which have been implicated in the progression of a variety of chronic, systemic conditions.
These disorders include various cancers; such as colorectal, pancreatic, prostate, and breast cancer, and other diseases like cardiovascular disease, diabetes, cognitive disorders, respiratory issues, and complications relating to pregnancy.
The DNA ConneXions® Oral test panel identifies bacteria, viruses, fungi and parasites in removed teeth, blood, tissue, dental implants, bone grafts or other biological samples. It identifies the presence of 88 different pathogens, including tetanus, botulism, diphtheria, HPV 16 and HPV 18, Candida albicans and more.
Using PCR, one of the most advanced tools in molecular biology today, specificity of this test is one in a trillion or greater and the sensitivity of the panel is the ability to detect the DNA of between 1 and 10 microbes.
DON’T GUESS. GET THE TEST.
Reference:
- Petersen PE, Bourgeois D, Ogawa H, et al. The global burden of oral diseases and risks to oral health. Bulletin of the World Health Organization | September (2005); 83 (9) https://www.scielosp.org/article/ssm/content/raw/?resource_ssm_path=/media/assets/bwho/v83n9/v83n9a11.pdf Accessed April 4, 2022
- Mayo Clinic. https://www.mayoclinic.org/healthy-lifestyle/adult-health/in-depth/dental/art-20047475 Accessed April 4, 2022
- Grau AJ, Becher H, Ziegler CM, et al. Periodontal Disease as a Risk Factor for Ischemic Stroke. Stroke. (2004); Vol. 35, No. 2.:496-501.
- World Health Organization Fact Sheet Cardiovascular diseases (CVDs). https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds) Accessed April 4, 2022
- nhlbi.nih.gov Know the Differences Cardiovascular Disease, Heart Disease, Coronary Heart Disease
https://www.nhlbi.nih.gov/sites/default/files/media/docs/Fact_Sheet_Know_Diff_Design.508_pdf.
Accessed April 4, 2022
- Center for Disease Control and Prevention. https://www.cdc.gov/nchs/fastats/heart-disease.htm Accessed April 4, 2022
- Center for Disease Control and Prevention. https://www.cdc.gov/heartdisease/facts.htm Accessed April 4, 2022
- Periodontal (Gum) Disease – Causes, Symptoms, and Treatments. https://www.nidcr.nih.gov/sites/default/files/2017-09/periodontal-disease_0.pdf Accessed April 6, 2022
- Liccardo D, Cannavo A, Spagnuolo G, et al. Periodontal Disease: A Risk Factor for Diabetes and Cardiovascular Disease. Int. J. Mol. Sci. (2019); 20(6), 1414
- Bains R, Bains VK, Lesions of endodontic origin: An emerging risk factor for coronary heart diseases. Indian Heart Journal.(2018) Vol 70 (3):S431-S434
- Barbosa-Ribeiro M, Arruda- Vaconcelos R, Louzada LM et al. Microbiological analysis of endodontically treated teeth with apical periodontitis before and after endodontic retreatment. Clinical Oral Investigations (2020) 25;2017-2027
- Lechner J, von Baehr V. Impact of Endodontically Treated Teeth on Systemic Diseases. Denitstry (2018) 8:476
- Bolukbasi N, Ozdemir T, Oksuz, et al. Bacteremia following dental implant surgery: Preliminary results. Med Oral Patol Oral Cir Bucal. (2012) Jan; 17(1): e69–e75.
- Estrich CG, Lipman RD, Araujo MWB. Dental amalgam restorations in a nationally representative sample of US population aged ≥15 years: NHANES 2011–2016. Journal of Public Health Dentistry. (2021) 1-4.
- Aftabi R, Jafari P, Pirzadeh-Ashraf M. Assessing the Environmental and Health Adverse Effects of Mercury Released From Dental Amalgam: A Literature Review. Journal of Advances in Environmental Health Research.(2021); 9(2):91-104.
- Becher R, Wellendorf H, Sakhi AK, et al. Presence and leaching of bisphenol a (BPA) from dental materials, Acta Biomaterialia Odontologica Scandinavica,(2018) 4:1, 56-62,